Hammer Toe Producing Knee Pain
Overview
The smallest four toes of each foot have three bony segments connected by two joints. Hammertoe is a deformity in which one or more of the small toes develops a bend at the joint between the first and second segments. The tip of the toe turns downward, making it look like a hammer or claw. The second toe is the one most often affected. Hammertoe may be more likely to occur when the second toe is longer than the first toe or when the arch of the foot is flat.
Causes
Factors that may increase you risk of hammertoe and mallet toe include age. The risk of hammertoe and mallet toe increases with age. Your sex. Women are much more likely to develop hammertoe or mallet toe than are men. Toe length. If your second toe is longer than your big toe, it's at higher risk of hammertoe or mallet toe. 
Symptoms
For some people, a hammer toe is nothing more than an unsightly deformity that detracts from the appearance of the foot. However, discomfort may develop if a corn or callus develops on the end or top of the toe. If pressure and friction continue on the end or top of the toe, a painful ulcer may develop. Discomfort or pain can lead to difficulty walking.
Diagnosis
Although hammertoes are readily apparent, to arrive at a diagnosis the foot and ankle surgeon will obtain a thorough history of your symptoms and examine your foot. During the physical examination, the doctor may attempt to reproduce your symptoms by manipulating your foot and will study the contractures of the toes. In addition, the foot and ankle surgeon may take x-rays to determine the degree of the deformities and assess any changes that may have occurred.
Non Surgical Treatment
There are many non-surgical treatments to help relieve symptoms of hammertoe. The first step for many people is wearing the right size and type of shoe. Low-heeled shoes with a boxy or roomy toe area are helpful. Cushioned insoles, customized orthopedic inserts, and pads can provided relief as well. Splints or straps may be used to help correct toe position. Your doctor may show you toe stretches and exercises to perform. Your doctor can safely remove corns and calluses. You should not try to remove them at home.
Surgical Treatment
In more advanced cases of hammer toe, or when the accompanying pain cannot be relieved by conservative treatment, surgery may be required. Different types of surgical procedures are performed to correct hammer toe, depending on the location and extent of the problem. Surgical treatment is generally effective for both flexible and fixed (rigid) forms of hammer toe. Recurrence following surgery may develop in persons with flexible hammer toe, particularly if they resume wearing poorly-fitted shoes after the deformity is corrected.
What Are The Symptoms Of Bunions?
Overview
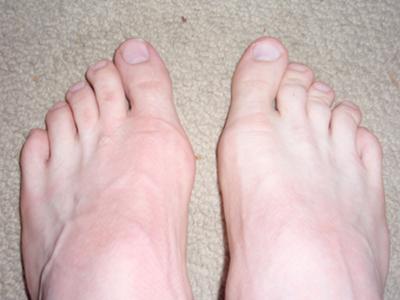 When the big toe is misaligned, it creates an unnatural bump on the inside of the forefoot (see image below). In addition to being unsightly, the lump or bunion can cause pain and make buying shoes difficult. Some people are born predisposed to bunions. But most people acquire them over time from ill-fitting footwear that squeezes the big toe inward toward the other toes. About four out of five bunion pain patients are female, a near perfect fit for the bad shoe theory. The good news, Bunions can be corrected, often with better-fitting shoes and custom orthotics. There are also some cases that cause severe bunion pain and do not respond to conservative treatment. For those patients, bunion surgery called bunionectomy may be necessary.
When the big toe is misaligned, it creates an unnatural bump on the inside of the forefoot (see image below). In addition to being unsightly, the lump or bunion can cause pain and make buying shoes difficult. Some people are born predisposed to bunions. But most people acquire them over time from ill-fitting footwear that squeezes the big toe inward toward the other toes. About four out of five bunion pain patients are female, a near perfect fit for the bad shoe theory. The good news, Bunions can be corrected, often with better-fitting shoes and custom orthotics. There are also some cases that cause severe bunion pain and do not respond to conservative treatment. For those patients, bunion surgery called bunionectomy may be necessary.
Causes
Despite the popular belief, wearing high heels and too-narrow shoes does not cause bunions. Wearing them can irritate, aggravate, or accelerate the formation of the bunion, but are not the root cause. Bunions are more commonly inherited, if your parents or grandparents had bunions, you may also get one. Bunions can also be caused by trauma or injury to the joints, ligaments, or bones of the foot.
Symptoms
Bunions may or may not cause symptoms. A frequent symptom is foot pain in the involved area when walking or wearing shoes that is relieved by resting. A bunion causes enlargement of the base of the big toe and is usually associated with positioning of the big toe toward the smaller toes. This leads to intermittent or chronic pain at the base of the big toe. Bunions that cause marked pain are often associated with swelling of the soft tissues, redness, and local tenderness. It is important to note that, in post-pubertal men and post-menopausal women, pain at the base of the big toe can be caused by gout and gouty arthritis that is similar to the pain caused by bunions.
Diagnosis
A doctor can very often diagnose a bunion by looking at it. A foot x-ray can show an abnormal angle between the big toe and the foot. In some cases, arthritis may also be seen.
Non Surgical Treatment
Apply special pads and dressings to protect the bunion from shoe pressure. Inject steroid and local anesthetic around the bunion to reduce inflammation. This is especially useful if there is an associated bursitis. Recommend commercially available or custom made shoes. Prescribe functional orthotics to correct faulty foot function, and help prevent worsening of the deformity. Recommend bunion surgery to correct the deformity. 
Surgical Treatment
Surgical treatment for bunion deformities usually involves an osteotomy, a procedure in which a cut or cuts are made in the affected bone or bones to restore proper alignment. Different techniques are used depending on the type of deformity; selection is guided by the degree of deformity present and the goals of preventing recurrence and achieving the most rapid recovery possible. Some of the more common procedures are. The distal chevron osteotomy: a procedure in which a v-shaped cut is made at the toe end of the first metatarsal. This surgery is appropriate for individuals who have a congruent deformity, one in which there is a painful prominence at the base of the toe, but the joint is still well aligned. Absorbable pins are placed in the metatarsal to maintain alignment during healing. The Scarf or Ludloff osteotomy: in this procedure, a more extensive cut is made higher up in the metatarsal to correct a moderate incongruent deformity and metatarsus primus varus. Screws are used to maintain alignment during healing. The crescent osteotomy: a procedure in which a curved cut is made at the base of the metatarsal is appropriate for patients with more severe metatarsus primus varus and, therefore, require more correction. Screws or pins are used to maintain alignment. The Lapidus procedure: individuals who have severe deformity, instability of the first ray, with a loose metatarsal-tarsal joint (located in the mid-foot) may not get enough correction from an osteotomy alone. Moreover, the looseness of the joint may lead to recurrence or be causing pain on the ball of the foot because the first metatarsal is floating up, allowing for excessive weight to go to adjacent metatarsals (commonly the second and the third). In such cases, the metatarsal-tarsus joint is fused to provide lasting stability. Screws are used to maintain alignment. The loss of motion from the fusion is small and does not significantly limit motion of the big toe. Patients undergoing bunion surgery are given an ankle block that anesthetizes the foot from the ankle down. Depending on individual preference, a sedative may be given as well and the patient can be as sedated as they wish. All bunion surgeries may be done on a same-day basis, eliminating the need for hospitalization.